InSee
Smart Incentive Spirometry System
Better compliance for better outcomes

What is InSee?
Enhancing Compliance to Reduce Post-Op Pulmonary Complications
Post-operative pulmonary complications (PPCs) are a serious concern, with clinical studies showing PPC rates as high as 50% in high-risk surgeries. These complications can add an average of 7.9 days to hospital stays and increase healthcare costs by $40,000 per patient. However, research has also demonstrated that compliant incentive spirometry (IS) can reduce PPC rates by 33% and shorten hospital stays by two days compared to patients who do not use IS.
Despite these benefits, the main challenge with incentive spirometry is poor patient compliance—both in performing lung exercises and achieving tidal volume goals. Studies have shown that adding a simple patient reminder can improve IS compliance by 106% and reduce ICU stay by one day.
InSee is a programmable smart sensor that attaches to existing incentive spirometers to address these compliance challenges. It delivers audible and visual reminders to encourage patients to perform their IS exercises consistently and correctly, helping to improve outcomes and reduce the risk of post-op pulmonary complications.
A survey of clinicians found that 86% believe patient adherence to IS is poor, and 95% agree that adherence should be improved. Studies have demonstrated that incorporating “nurse guidance” and “patient reminders” significantly increases compliance, leading to fewer cases of atelectasis, reduced hypoxic events, and shorter ICU stays.
With InSee, a patient’s Respiratory Therapist or Nurse can program individualized tidal volume and repetition goals. InSee then coaches the patient with real-time reminders to ensure compliance. Additionally, InSee tracks max tidal volume and usage frequency, providing clinicians with objective data to guide intervention and optimize recovery.
By monitoring and reinforcing consistent usage of the incentive spirometer, the InSee Smart Incentive Spirometry System enables better post-operative pulmonary outcomes, shorter hospital stays, and reduced healthcare costs—without requiring constant provider oversight.
.png)
Request a Free InSee
You now can trial the InSee in your hospital at no cost
Proven Methods to Improve Incentive Spirometry
Incorporating Smart Patient Reminders & Objective Monitoring
One of the primary challenges with Incentive Spirmetery is ensuring patient compliance with the therapy. In a comprehensive survey, 86% of clinicians* believed that patient adherence to traditional incentive spirometry exercises is poor, and 95% believed that incentive spirometry exercises adherence should be improved. Patients are required to use their incentive spirometers five to ten times an hour by taking deep breaths and sustaining certain lung volumes. Clinical studies have demonstrated that incorporating patient reminders with incentive spirometry and monitoring patient usage can improve patient adherence and outcomes.
Clinically Proven
Adding Patient Reminder Alarms to Incentive Spirometry Improved Patient Outcomes
In a 2019 study published in Jama Surgery, adding a reminder alarm to incentive spirometry showed to improve post-cardiac surgery patients' outcomes. In this randomized clinical trial 160 participants, who underwent nonelective CABG, were randomized, with 145 completing the study per protocol. A use-tracking, IS add-on device with an integrated use reminder bell recorded and timestamped participants’ inspiratory breaths. Patients were randomized by hourly reminder “bell-on” (experimental group) or “bell-off” (control group). With 74 (51.0%) in the bell-off group and 71 in the bell-on group.
The incentive spirometer reminder improved patient adherence, atelectasis severity, early postoperative fever duration, noninvasive positive pressure ventilation use, ICU and length of stay, and 6-month mortality in certain patients. With the reminder, IS appears to be clinically effective when used appropriately. Detailed outcomes are as follows:
-
Improved mean daily inspiratory breaths (35.4 vs 17.1;P < .001)
-
Reduced mean atelectasis severity (1.5 vs 1.8; P = .04)
-
Reduced noninvasive positive pressure ventilation use rates (37% vs 19%; P = .03)²
-
Reduced pneumonia (5%vs 1%; P = .18)
-
Reduced postoperative length of stay (7 vs 6 days; P = .048)²
-
Reduced the ICU length of stay (4 vs 3 days; P = .02)²
-
Reduced deaths at 6 months (0%vs 9%; P = .048)²
-
Reduced fever duration (3.2 hours; 95%CI, 2.3-4.6 vs 5.2 hours; 95%CI, 3.9-7.0; P = .04).
Nurse-guided Use of Incentive Spirometry Improved Patient Outcomes
Nurse-guided use of Incentive Spirometry reduces the risk of post-pulmonary complications and hospital length of stay after cardiac surgery. In a 2020 study published in the International Journal of Nursing Practice, a total of 89 patients were randomized into either control or intervention groups. Patients in the intervention group received bi-hourly nurse-guided incentive spirometry for 48-h postextubation. Patients in the intervention group had a significantly lower mean number of hypoxic events with shorter duration and shorter lengths of stay in the hospital and the ICU.
Detailed outcomes are as follows:
-
Reduced number of Hypoxic events: 9.4 vs 30.9, P<0.001
-
Reduced duration of Hypoxic events: 36min vs 176min , P<0.001
-
Reduced post-op Hospital length of stay: 8.6 vs 12, P= 0.02
-
Reduced post-op ICU length of stay 1.8 vs 12., P<0.001
-
Reduced incidents of Pneumonia: 17.9% vs 2.6%
InSee Features & Benefits
Smart Patient Coaching
Help promote patient compliance and better outcomes.
Continuous Patient Monitoring
Identify high risk patients & imrpove staff workflow.
Risk
Stratification
Early detection to lower length of stay & readmissions.
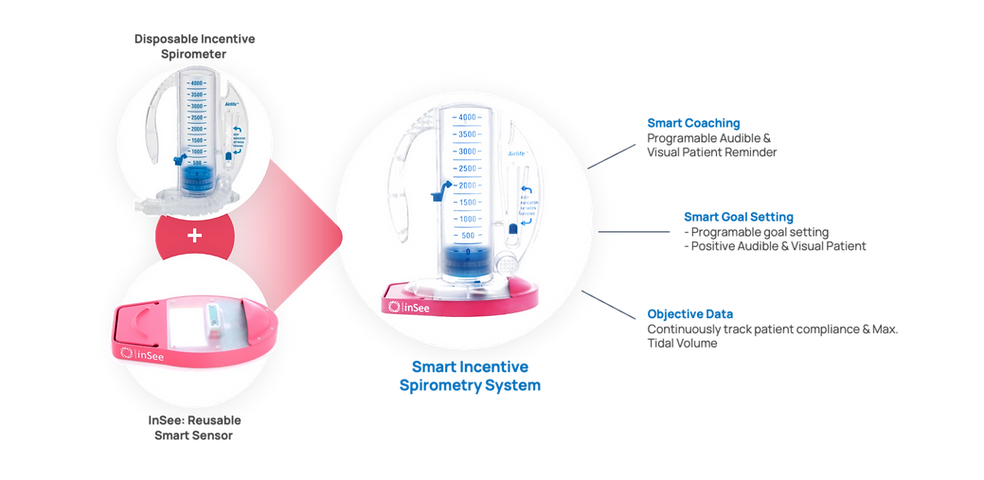
Smart Patient Coaching & Goal Setting
During the introduction of traditional Incentive Spirometry (IS), a Respiratory Therapist or Nurse sets the patient's goal volume on the device and instructs the patient to inhale via the IS tube until the piston reaches the goal volume. Patients are instructed to repeat this procedure five to ten times every hour. However, it is well known that not only patients do not use the IS as often as they are instructed to, but they also barely reach the preset goal volume.
With InSee, the Respiratory Therapist or Nurse configures the desired goal volume and inhalation cadence. Then throughout the day, the InSee alarm reminds the patient to use the IS per the preconfigured cadence. Also with every inhalation, if the patient reaches the goal volume, the InSee illuminates a green light to let the patient know they successfully reached the goal, thus providing positive reinforcement and motivation. InSee's Smart Patient Coaching feature encourages more frequent and consistent usage of the incentive spirometer, without reliance on the presence of the healthcare provider or reliance on the patient's memory
Continuous Patient Monitoring
Incentive spirometry is most effective when used consistently and in conjunction with proper monitoring by healthcare professionals. However, due to resource constraints or patient factors, regular monitoring may not always be feasible. Currently, patients self-report their Inventive Spirometry compliance level which is not a reliable method to measure the treatment efficacy.
The InSee continously tracks the number of patient inhalation attempts, the number of times the goal volume was successfully reached, and the max tidal volume.
Risk Stratification
Tidal volume, which refers to the volume of air inspired or expired with each normal breath during spontaneous breathing, plays an important role in postoperative pulmonary complications (PPCs), including atelectasis and pneumonia, risk-stratification. The appropriate management of tidal volume is crucial in the post-operative period to reduce the risk of respiratory complications and improve patient outcomes.
The InSee tracks the patients' tidal volume continuously which allows clinicians to identify the patients at higher risk and implement early interventions before the patient's condition is worsened.
.png)
CASE STUDY: 300% Improvement
InSee shown to improve max tidal volume in patient hospitalized with Septic Shock
Hospital: River Oak Hospital. Houston, TX
Background: A male patient had been hospitalized due to Septic Shock at River Oak Hospital for ten days. Despite all efforts with regular Incentive Spirometry (IS), the patient’s Max Tidal Volume remained at 500cc using the Incentive Spirometer (IS) alone. On the day the InSee was introduced to the Respiratory Care department, one of the Respiratory Therapists suggested starting this patient on InSee immediately.
Results: Within two days of IS+InSee, the patient’s Max Tidal Volume increased to 750cc and within four days it reached 1500cc
Observation: The InSee reminder engaged the patient, caregivers, nurses, & techs to reinforce IS usages which resulted in significant improvement in Max Tidal Volume. In addition to improved breathing, the patient’s mood consciously improved. Continuous improvement, positive re-enforcement, and engagement helped the patient’s overall health and motivation.

FDA & Regulatory Status
The InSee has been identified as a Non-significant Risk device that allows healthcare professionals to trial the system while awaiting 510K clearance. The InSee is expected to receive FDA 510K clearance in 2024.
In June of 2021, the U.S. Food and Drug Administration (FDA) issued an Emergency Use Authorization (EUA) for emergency use of the InSee incentive spirometer accessory for quantitatively tracking patient usage of Vyaire Medical’s AirLife incentive spirometer, as an aid in the treatment of respiratory conditions.
If you are interested to use the InSee in your hospital, complete the form below.
Incentive Spirometry vs Spirometry
Incentive Spirometry vs. Oscillating Positive Expiratory:
The main difference between incentive spirometry and oscillating positive expiratory pressure devices lies in their mechanisms of action and clinical applications. Incentive spirometry focuses on lung expansion and prevention of atelectasis, primarily in the post-operative setting. On the other hand, oscillating positive expiratory pressure devices, such as Aerobika, are designed to facilitate mucus clearance and airway hygiene in patients with chronic respiratory conditions. While both therapies aim to improve lung function and respiratory outcomes, they are used in different patient populations and clinical scenarios.
Incentive Spirometry vs. Spirometry:
While both devices serve important roles in respiratory care, they are used for different purposes and in distinct clinical scenarios. Spirometers are diagnostic tools used to assess lung function and diagnose respiratory conditions, while incentive spirometers are therapeutic devices used to encourage deep breathing and lung expansion, particularly for the prevention and management of atelectasis, pneumonia, and other post-operative pulmonary complications. Spirometers provide objective measurements for diagnostic and monitoring purposes, while incentive spirometers are part of a patient's therapy to improve lung function and prevent complications.
Smart Incentive Spirometry:
The InSee Smart Incentive Spirometry System enhances the function of IS in two ways. First, it improves the therapeutic outcomes of incentive spirometry by improving patient adherence. Second, it elevates the IS into a diagnostic and monitoring by recoding patient compliance and max tidal volume continuously, which helps clinicians identify high-risk patients.

